Cutaneous aspergillosis in an immunocompetent patient: a case report
Abstract
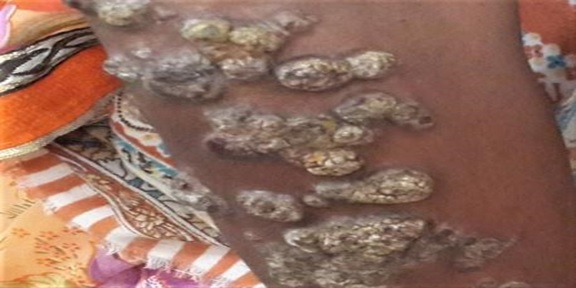
Cutaneous aspergillosis is a rare disease that is usually seen in immunosuppressed patients. It is rarely found in immunocompetent patients and it is mostly caused by Aspergillus. flavus, Aspergillus fumigatus, and rarely by Aspergillus niger. Cutaneous Aspergillosis is of two types: primary or secondary. Primary cutaneous aspergillosis frequently involves sites of skin injury, at or near intravenous catheter sites, at sites associated with occlusive dressings, at sites of traumatic inoculation, surgery or burns. Secondary cutaneous lesions occur as a result of either from widespread blood-borne seeding of the skin or it may occur from contiguous extension to the skin from an infected underlying structure. The current study is presenting a case of a 25-year-old female, a farmer by occupation, presented with multiple scaly plaques and verrucous nodules with a past history of trauma over knee 3 years back. After trauma she initially noticed lesions over knee followed by the elbow, face and oral lesions noticed 7 months back. There was no present or past history of weight loss, anorexia and serological tests were negative for HIV. One year back she was diagnosed as lupus vulgaris and received Anti-Tubercular treatment without much benefit. She came to our hospital where biopsy from lesions over elbow revealed dense inflammatory exudate, septate fungal hyphae showing acute angle branching on H and E stain and PAS stain, which is suggestive of aspergillosis. Scrapping from oral lesion also revealed inflammatory cells with septate fungal hyphae with acute angle branching on PAP stain. Histopathological, cytological study and fungal culture show fungal infection caused by Aspergillus niger. In cutaneous aspergillosis, surgical excision alone or combination with drug therapy was found to be curative. The present case report was important due to its rarity.
Downloads
References
Jagdish Chander. Textbook of Medical Mycology.4th edition. Haryana: Jaypee,2018, page no.524- 553.
Tahir C, Garbati M, Nggada HA, Yawe EHT, Abubakar AM. Primary cutaneous aspergillosis in an immunocompetent patient. J Surg Tech Case Rep. 2011;3(2):94-96. doi: https://doi.org/10.4103/2006-8808.92802.
Khatri ML, Stefanato CM, Benghazeil M, Shafi M, Kubba A, Bhawan J. Cutaneous and paranasal aspergillosis in an immunocompetent patient. Int J Dermatol. 2000;39(11):853-856.
Xess I, Swetha J, Tanveer N, Asati D, Ramam M, Singh M, et al. Primary cutaneous aspergillosis due to Aspergillus niger in an immunocompetent patient. Indian J Med Microbiol. 2009;27(4):367-370. doi: https://doi.org/10.4103/0255-0857.55462.
Chakrabarti A, Gupta V, Biswas G, Kumar B, Sakhuja VK. Primary cutaneous aspergillosis: Our experience in 10 years. J Infect. 1998;37(1):24-27. doi: https://doi.org/10.1016/S0163-4453(98)90303-6.
Sharma S, Yenigalla BM, Naidu SK, Pidakala P. Primary cutaneous aspergillosis due to Aspergillus tamarii in an immunocompetent host. BMJ Case Rep. 2013. doi: https://doi.org/10.1136/bcr-2013-010128.
Chong YS, Ro BI. Cutaneous aspergillosis. Korean J Med Mycol. 2002;7(1):6-13. doi: https://doi.org/10.1007/3-540-29668-9_700.
Granstein RD, First LR, Sober AJ. Primary cutaneous aspergillosis in a premature neonate. Br J Dermatol. 1980;103(6):681-684. doi: https://doi.org/10.1111/j.1365-2133.1980.tb01693.x.
Venugopal T V., Venugopal P V. Primary cutaneous aspergillosis from Tamilnadu diagnosed by fine needle aspiration cytology. Med Mycol Case Rep. 2012;1(1):103-106. doi: https://doi.org/10.1016/j.mmcr.2012.09.004.
Xiaoyan Liu, Jun Yang, Weiyuan Ma. Primary cutaneous aspergillosis caused by Aspergillus. fumigatus in an immunocompetent patient. Medicine (United States).2017;96(48):56-59. doi: https://doi.org/10.1097/MD.0000000000008916.
Camus M, Anyfantakis V, Dammak A, Riche A, Delouane H, Roblot F, et al. Aspergillose cutanée primitive chez un agriculteur immunocompétent. Ann Dermatol Venereol. 2010;137(5):373-376. doi: https://doi.org/10.1016/j.annder.2010.03.006.
Singh SG, Singh T, Neki N, Singh A, Bans Sidhu P, Singh Pannu J. cutaneous Aspergillosis in an immunocompetent patient. Int J Med Health Res. 2016;2(12):57-58.
Prasad PVS, Babu A, Kaviarasan PK, Anandhi C, Viswanathan P. Primary cutaneous aspergillosis. Indian J Dermatol, Venereol Leprol. 2005;71(2):133-134. doi: https://doi.org/10.4103/0378-6323.14006.
Woodruff CA, Herbert AA. Neonatal primary cutaneous aspergillosis: Case report and review of the literature. Pediatric Dermatol.2002;19(5):439-444. doi: https://doi.org/10.1046/j.1525-1470.2002.00203.x.
Stevens DA, Kan VL, Judson MA, Morrison VA, Dummer S, Denning DW, et al. Practice Guidelines for Diseases Caused by Aspergillus. Clin Infect Dis.2000;30(4):696-709. doi: https://doi.org/10.1086/313756.
Romano C, Miracco C. Primary cutaneous aspergillosis in an immunocompetent patient. Mycoses. 2003;46[1–2]:56–9. doi: https://doi.org/10.1046/j.1439-0507.2003.00836.x.
van Burik JA, Colven R, Spach DH. Cutaneous aspergillus. J Clin Microbiol.1998;36(11):3115-3121.
Ajith C, Dogra S, Radotra BD, Chakrabarti A. Primary cutaneous aspergillosis in an immunocompetent individual. J Eur Acad Dermatol Venerol.2006;20(6):738-739. doi: https://doi.org/10.1111/j.1468-3083.2006.01465.x.
Avkan-Oğuz V, Çelik M, Satoglu IS, Ergon MC, emrah Açan A. Primary Cutaneous Aspergillosis in Immunocompetent Adults: Three Cases and a Review of the Literature. Cureus 2020;12(1):e6600. doi: https://doi.org/10.7759/cureus.6600.
Copyright (c) 2020 Author (s). Published by Siddharth Health Research and Social Welfare Society

This work is licensed under a Creative Commons Attribution 4.0 International License.


 OAI - Open Archives Initiative
OAI - Open Archives Initiative


