A rare mesentric tumor “paraganglioma” – a case report
Abstract
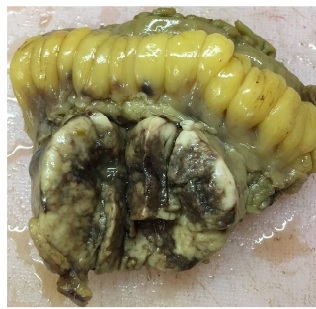
Paraganglioma are rare type of neuroendocrine tumors that arise from embryonal neural crest. Paraganglioma of adrenal medulla is known as Pheochromocytoma. Extra adrenal localization has incidence of 2-8 per million people per year, which can extend from upper cervical region to pelvis related to autonomic nervous system. Even rarer is occurrence of paragangliomas outside the usual distribution of paraganglionic tissue. Mesenteric paragangliomas are extremely rare. The present case was of a non-functional extra adrenal paraganglioma occurring in a 43-year-old male presented with complain of pain in abdomen and mild discomfort. Abdominal CECT revealed well defined enhancing solid mass with central necrosis in right side of mesentry. Explorative laparotomy and surgical excision were done, on histology typical “zellballen” pattern was found. Paragangliomas are rare neuroendocrine tumor known to store and secrete catecholamines and hence are known as functional paragangliomas and may present with symptoms like headache, sweating, palpitations and hypertension. On other hand, they may remain silent and non-functional and present with vague symptoms like pain abdomen due to episodic release of catecholamines. Surgical excision is treatment of choice. Long term follow up is mandatory as tumor is prone to recur and metastasize.
Downloads
References
2. Hemalatha AL, Avadhani Geeta K., Anoosha K, Ashok KP, Extra-adrenal silent retroperitoneal paraganglioma: Report of a rare case. Journal of clinical and diagnostic research: JCDR 2014;8(11):FD06-FD07. doi: https://dx.doi.org/10.7860%2FJCDR%2F2014%2F10133.5138.
3. Cherit M, Dube P, Royal V, Leblanc G, Sideris L. Malignant paragangliomaof the mesentery: a case report and review of literature. Worls J Surg oncol. 2012;10:46. doi: https://doi.org/10.1186/1477-7819-10-46.
4. Lagorga JB, Vaquero M, Juanpere N, Paragastric Paraganglioma: A case report with Unusual Alveolar Pattern and Myoxid Component Cytopathol. 2012;40(9):815-819. doi: https://doi.org/10.1002/dc.21665
5. Pruiti V, Mazzeo F, Rossitto M, Foti A, Macri A, Cucinotta E, Gastric paraganglioma: A case report and a review of the literature. Ann Ital Chir. 2014;29:85.
6. Crosbie L, Humphreys WG, Maxwell M, Maxwell P, Cameron CHs, Toner PG, Castric paraganglioma: an immunohistological and ultrastructural case study. J Submicrosc Cytol Pathol. 1990;22(3):401-408.
7. Buonuomo V, Ruggiero A, Rando G, D’urzo C, Manzoni C, pintus C, Malignant retroperitoneal paraganglioma: case report and review of the literature. Pediatr Hematol Oncol. 2004;21(8):731-738. doi: https://doi.org/10.1080/08880010490515029.
8. Absher KJ, Witte DA, Trung LD, Ramzy I, Mody DR, Ostrowski ML. Aspiration biopsy of osseous metastasis of retroperitoneal paraganglioma: report of a case with cytologic features and differential diagnostic considerations. Actacytol. 2001;45(2):249-253. doi: https://doi.org/10.1159/000327284.
9. Offergeld C, Brase C, Yaremchuk S, Mader I, Rischke HC, Glasker S, et al. Head and neck paragangliomas: clinical and molecular genetic classification. Clinics 2012;67(1):19-28. https://doi.org/10.6061/clinics/2012(sup01)05.
10. Perrot G, Pavic M, Mitou F, Crozes C, Faucompret S, Vincent E, diagnostic difficile d’un paragangliomepancreatuque. Rev Med Interne 2007;28(10):701-704. doi: https://doi.org/10.1016/j.revmed.2007.06.001.
11. Kinney Ma, Narr BJ, Warner MA. Perioperative management of pheochromocyta,. J Cardiothorac Vasc Anesth. 2002;16(3):395-369. doi: https://doi.org/10.1053/jcan.2002.124150.
12. Vanderveen Ka, Thompsan SM, Callstrom Mr, Young WF, Jr, Grant CS, Farley DR, Richards ML, Thompson GB. Biopsy of pheochroocytomas and paraganglioma potential for disaster. Surg. 2009;146(6):1158-1166. doi: https://doi.org/10.1016/j.surg.2009.09.013.
13. Belhamidi MS, Ratbi MB, Tarchouli M, Adioui T, Ali AA, Zentar A Sair K. An unusual localization of retroperitoneal paraganglioma: a case report. Pan Af Med J. 2015;22(1):12. doi: https://dx.doi.org/10.11604%2Fpamj.2015.22.12.7437.
14. Wen J, LI HZ, Ji ZG, Mao QZ, Shi BB, Yan WG. A decade of clinical experience with extra-adrenal paragangliomas of retroperitoneuml Report of 67 cases and a literature review. Urol Ann. 2010;2(1):12-16. doi: https://dx.doi.org/10.4103%2F0974-7796.62919.
15. Chrisoulidou A, Kaltsas G, Ilias I, Grossman AB. The diagnosis and management of malignant phaeochromocytoma and paraganglioma. Endocr Relat Cancer. 2007;14(3):569-585. doi: https://doi.org/10.1677/ERC-07-0074.
16. Shah U, Giubellino A, Pecak K. Pheochromocytoma: complications in tumorigenesis and the actual management> Minerva Endocrinol. 2012;37(2):141-156.
17. Sclafani LM, Woodruff JM, Brennan MF. Extraadrenal retroperitoneal paragangliomas: natural history and response to treatment. Surg. 1990;108(6):1124-1129.
Copyright (c) 2020 Author (s). Published by Siddharth Health Research and Social Welfare Society

This work is licensed under a Creative Commons Attribution 4.0 International License.


 OAI - Open Archives Initiative
OAI - Open Archives Initiative


